| Original Literature | Model OverView |
|---|---|
|
Publication
Title
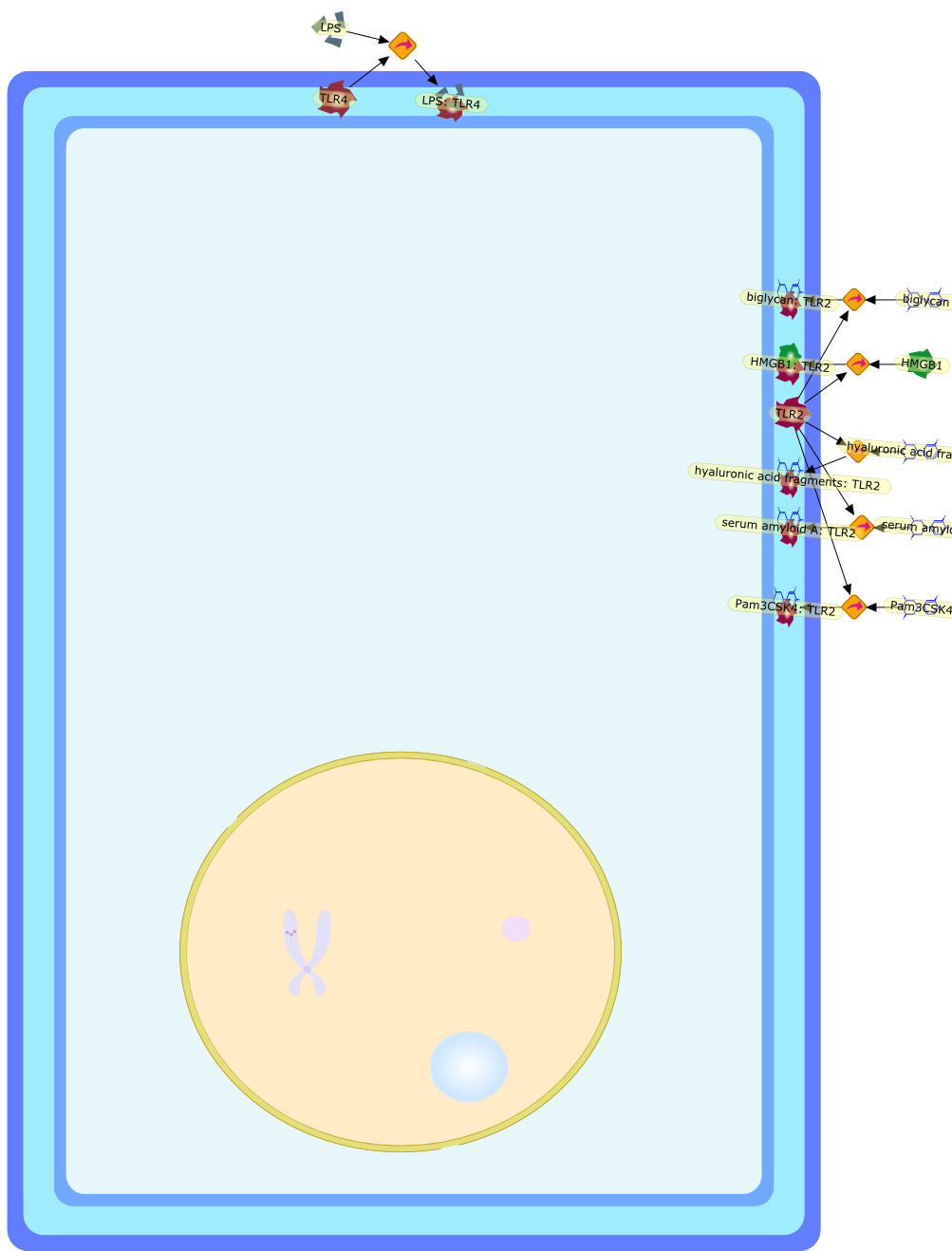
Toll-like receptors in atherosclerosis.
Affiliation
Department of Immunology, The Scripps Research Institute, 10550 North TorreyPines Road, La Jolla, CA 92037, USA.
Abstract
At one time, atherosclerosis was thought to be a simple lipid storage disease.However, it is now recognized as a chronic and progressive inflammation of thearterial wall. Gene deletion experiments in murine models of atherosclerosisthat reduce the inflammatory process also reduce disease severity. Identifyingthe initiators and mediators of that inflammation can provide promising avenuesfor prevention or therapy. Two prominent risk factors, hyperlipidaemia andinfectious disease, point to innate immune mechanisms as potential contributorsto proatherogenic inflammation. The TLRs (Toll-like receptors), pro-inflammatorysensors of pathogens, are potential links between inflammation, infectiousdisease and atherosclerosis. A mechanism for hyperlipidaemic initiation ofsterile inflammation can be postulated because oxidized lipoproteins or theircomponent oxidized lipids have been identified as TLR ligands. Moreover,infectious agents are correlated with atherosclerosis risk. We have identified arole for TLR2 in atherosclerosis in mice deficient in low-density lipoproteinreceptor. We observed that proatherogenic TLR2 responses to unknown endogenousor unknown endemic exogenous agonists are mediated by non-BMDC(bone-marrow-derived cells), which can include endothelial cells. In contrast,the proatherogenic TLR2 responses to the defined synthetic exogenous agonistPam3 CSK4 are mediated at least in part by BMDC, which can include lymphocytes,monocytes/macrophages and dendritic cells. TLR2-mediated cell activation inresponse to endogenous and exogenous agents is proatherogenic in hyperlipidaemicmice.
PMID
18031244
|